Why Choose TMS for OCD Treatment
Efficacy of TMS for OCD
Transcranial Magnetic Stimulation (TMS) is recognized for its effectiveness in treating Obsessive-Compulsive Disorder (OCD). In 2018, the Food and Drug Administration approved TMS specifically for OCD, particularly for individuals whose symptoms have not improved with traditional medication and psychotherapy options.
Recent research highlights the efficacy of TMS, especially low-frequency TMS, which targets key brain regions like the dorsolateral prefrontal cortex and supplementary motor area. A 2021 review indicates that this targeted approach is effective in alleviating OCD symptoms.
The success rates for TMS in treating OCD symptoms are promising, with numerous studies suggesting that the majority of patients experience significant symptom reduction after a course of treatment. For an overview of patient experiences, check out our section on success stories with TMS.
| Study | Effectiveness Rating |
|---|---|
| rTMS on DLPFC | High |
| dTMS on mPFC | Moderate |
| rTMS on SMA | Moderate |
FDA Approval and Safety of TMS for OCD
The FDA’s approval of TMS for OCD underscores its safety and reliability as a treatment option. TMS therapy is considered safe and well-tolerated, with no severe side effects such as memory loss or seizures reported. Unlike many other treatment modalities, TMS does not require anesthesia, making it a more accessible alternative for patients [2].
Most patients tolerate TMS well, experiencing only mild side effects such as temporary headache or scalp discomfort, which typically subside shortly after the session. TMS offers a non-invasive, drug-free solution to managing OCD, making it an attractive choice for those seeking alternatives to conventional antidepressants and psychotherapy.
To explore further treatment options, including drug-free alternatives, visit our page on non-invasive depression treatment.
For a more comprehensive understanding of TMS and its impact on OCD, refer to our sections on TMS therapy provider and who qualifies for TMS therapy.
TMS Treatment Details
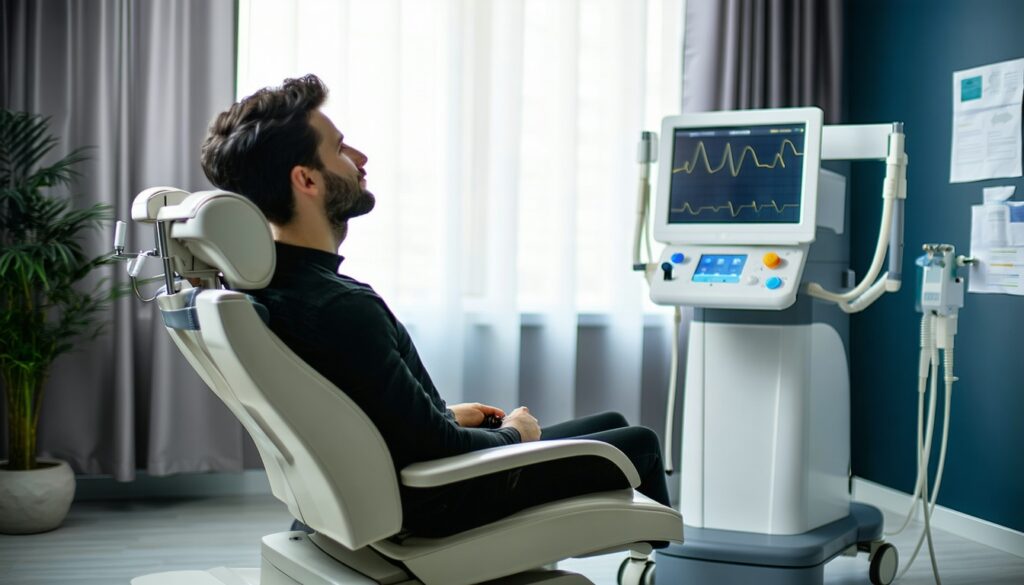
Understanding the specifics of TMS (Transcranial Magnetic Stimulation) for OCD will help you make informed decisions regarding your treatment options. This section covers session details, potential side effects, and the brain areas targeted during TMS therapy.
Duration and Frequency of Sessions
Typically, each TMS session for OCD lasts between 20 and 60 minutes, depending on individual treatment protocols and needs. Most patients undergo treatment several times a week over a span of about 4 to 6 weeks [1].
| Treatment Component | Frequency | Duration |
|---|---|---|
| Initial Sessions | 3-5 times per week | 20-60 minutes |
| Total Treatment Duration | 4-6 weeks | Varies according to protocol |
Regular attendance is crucial for achieving optimal results. Familiarizing yourself with these time commitments can help you plan accordingly.
Side Effects and Tolerability
TMS is generally well-tolerated, with few patients reporting side effects. Commonly reported side effects include mild discomfort at the treatment site, headache, or fatigue immediately following a session. These effects are typically temporary and resolve shortly after treatment.
| Side Effect | Description |
|---|---|
| Local Discomfort | Mild tingling or pressure at the site of stimulation |
| Headache | Short-lived and often manageable with over-the-counter pain relief |
| Fatigue | Temporary drowsiness that can follow a session |
Most individuals find TMS to be a preferable alternative to traditional treatments such as medication, especially considering its non-invasive nature. For more insight on tolerability, refer to our article on TMS side effects and results.
Specific Brain Targets for OCD Treatment
TMS therapy specifically aims at brain regions associated with OCD, primarily the prefrontal cortex, supplementary motor area, and orbitofrontal cortex. Targeting these areas promotes the release of neurotransmitters like serotonin and dopamine, which can help alleviate OCD symptoms by restoring neurological balance. Each TMS session efficiently stimulates these areas, encouraging neuronal activity vital for mood regulation and anxiety control [3].
Increasingly, practitioners may employ higher frequencies or more intense stimulation parameters during treatment to enhance efficacy. If you’re curious to learn more about how TMS works, visit our article on how does TMS therapy work.
By understanding the treatment cycle, potential side effects, and the targeted brain areas, you gain a clearer perspective on how TMS for OCD can help.
Comparing TMS Variants
When considering TMS for OCD, understanding the different variants of transcranial magnetic stimulation (TMS) can help you make an informed decision. This section will explore the distinctions between rTMS and dTMS, the effects of excitatory versus inhibitory TMS, and the usage of theta burst stimulation (TBS) protocols.
rTMS vs dTMS for OCD
Repetitive transcranial magnetic stimulation (rTMS) and deep transcranial magnetic stimulation (dTMS) are both neuromodulation techniques used to treat OCD.
| Feature | rTMS | dTMS |
|---|---|---|
| Depth of Penetration | Moderate | Deeper |
| Target Area | Specifically focused areas | Broader coverage |
| Treatment Type | Usually used in outpatient settings | May require specialized equipment |
According to PubMed Central, both rTMS and dTMS can be effective as add-on treatments alongside pharmacological interventions. While rTMS targets specific areas such as the supplementary motor area (SMA) or orbitofrontal cortex, dTMS may provide deeper stimulation to affect a larger area of the brain.
Excitatory vs Inhibitory TMS Effects
In the context of OCD treatment, TMS can be categorized based on its effects on brain activity: excitatory and inhibitory.
| Type of TMS | Effect | Frequency |
|---|---|---|
| High-frequency rTMS | Excitatory | Used to increase cortical activity |
| Low-frequency rTMS | Inhibitory | Used to decrease cortical activity |
According to research, low-frequency rTMS is typically associated with inhibitory effects, while high-frequency rTMS is seen as excitatory. Additionally, theta burst stimulation (TBS) protocols have emerged, with continuous TBS (cTBS) producing inhibition and intermittent TBS (iTBS) leading to excitation.
TBS Protocols for OCD
Theta burst stimulation is a newer protocol that has shown promise in treating OCD symptoms. TBS delivers bursts of stimulation, which can influence brain activity in a way analogous to traditional sessions while potentially reducing the overall treatment time.
| TBS Type | Effect | Duration |
|---|---|---|
| cTBS | Inhibitory | Shorter sessions with repeated bursts |
| iTBS | Excitatory | Similar to cTBS but aims to stimulate activity |
These TBS protocols allow for shorter treatment sessions with similar efficacy to traditional rTMS methods. Studies have indicated the potential for effective outcomes using TBS in managing OCD symptoms. For more on how TMS works, check our article on how does TMS therapy work.
Choosing the right TMS variant is crucial for effective treatment of OCD. Each approach offers unique benefits, and your treatment provider, like MindHealth MD, will work with you to identify the most suitable option based on your needs.
Success Stories with TMS
Patient Experiences with TMS
Numerous individuals have shared their experiences with TMS for OCD and expressed how transformative this treatment has been in their lives. Many patients report significant reductions in their OCD symptoms, which can include intrusive thoughts, compulsive behaviors, and anxiety. For those who have not found relief from traditional treatments like medication or psychotherapy, TMS has offered a beacon of hope.
For example, one patient described how their obsessive thoughts that once consumed their daily life became manageable after a series of TMS sessions. They noted that the therapy allowed them to engage more fully in their relationships and daily activities, ultimately improving their overall quality of life. Such testimonies highlight the potential for TMS to serve as a viable alternative for those facing treatment-resistant OCD.
Effectiveness of TMS on OCD Symptoms
Studies indicate that TMS can be particularly beneficial for individuals struggling with OCD who have not responded to conventional treatments. When applied as part of a comprehensive treatment strategy that includes psychotherapy, medication management, and lifestyle changes, TMS can produce remarkable results. Recent research shows that low-frequency rTMS targeting specific areas of the brain, such as the supplementary motor area (SMA) and orbitofrontal cortex, effectively reduces symptoms of OCD.
A notable statistic is that over 70% of individuals diagnosed with OCD may experience some degree of improvement in their symptoms through TMS treatment, providing a promising outlook for many seeking relief from their condition [5].
| Study Findings | Percentage of Improvement |
|---|---|
| Patients benefiting from traditional treatments | 70% |
| Patients experiencing success after TMS treatment | Variable, with many reporting significant reductions in symptoms |
Ultimately, the combination of TMS with other therapies often leads to the most effective results for managing OCD. It’s an innovative approach that continues to change lives and is worth considering if you or a loved one are exploring treatment options. If you wish to learn more about TMS treatment at your local provider, consider scheduling a first time TMS consultation for a personalized discussion.
Comprehensive Treatment Approach
In your journey to tackle OCD, understanding the most effective treatment strategies is vital. Transcranial Magnetic Stimulation (TMS) for OCD can yield significant benefits when combined with other therapies and lifestyle modifications.
TMS Combined with Other Therapies
Success with TMS for OCD often stems from integrating it with a multi-faceted treatment strategy. TMS is typically more effective when used alongside psychotherapy techniques like Cognitive-Behavioral Therapy (CBT) and Exposure and Response Prevention (ERP). Psychotherapy equips you with practical strategies to manage OCD symptoms while TMS addresses neurological aspects of the disorder. Medication management can also play a crucial role for some, enhancing overall treatment efficacy.
| Treatment Type | Description |
|---|---|
| TMS Therapy | Non-invasive neurostimulation focused on OCD |
| Cognitive-Behavioral Therapy | Psychological therapy focused on altering thought patterns |
| Exposure and Response Prevention | Controlled exposure to anxiety triggers to reduce responses |
| Medication Management | Use of prescribed medications as adjunct therapy |
By combining TMS with these approaches, you may experience a more comprehensive path toward recovery, especially if you are seeking alternatives after standard treatments have not yielded desired results.
Lifestyle Changes for Optimal Results
In addition to traditional treatments, incorporating specific lifestyle changes can significantly enhance the overall effectiveness of TMS and other OCD therapies. Key adjustments that may benefit you include:
- Stress Management Techniques: Practices like mindfulness, meditation, and yoga can help lower stress levels, which may exacerbate OCD symptoms.
- Regular Physical Activity: Engaging in regular exercise has been shown to reduce anxiety and depression, potentially improving mental health outcomes.
- Balanced Diet: Maintaining a nutritious diet can support overall well-being, impacting your mental health positively. Nutrients play a role in brain function, and a balanced diet can contribute to improved mood and cognition [3].
These lifestyle changes not only complement your TMS treatment but also foster a healthier, more balanced life, preparing you to engage more effectively in therapeutic practices. Consider these adjustments as part of your comprehensive treatment plan as you seek to manage OCD effectively.
Practical Considerations
Understanding the practical aspects of TMS therapy for OCD is crucial when deciding whether it’s the right option for you or a loved one. Here are essential factors to consider, including costs, treatment logistics, and success rates.
Cost Considerations for TMS Therapy
The cost of TMS therapy for OCD can vary significantly based on several factors, including symptom severity, location, and health insurance coverage. For those paying out of pocket, treatment costs may total at least $15,000. Insurance may cover the basic series of 30 treatments, although some plans require prior authorization or may necessitate trying other OCD treatments first.
| Cost Type | Estimated Amount |
|---|---|
| Out-of-Pocket Cost | $15,000+ |
| Insurance Coverage | Varies by plan |
It’s essential to check with your insurance provider to understand your coverage options and any out-of-pocket costs you might incur.
Outpatient Treatment and Convenience
TMS therapy is conducted as an outpatient service, which means you do not need to stay overnight at a facility. Treatments are typically scheduled five days a week, Monday through Friday, for six weeks, making it convenient to fit into your daily routine. Each session can last 3 to 10 minutes, making it a manageable commitment for individuals with busy lifestyles.
TMS Success Rates and Follow-up
The success rates of TMS therapy for OCD can vary, but many patients experience significant improvement in symptoms. Follow-up sessions may be recommended for continued effectiveness after the initial treatment course. Insurance may also cover “preservation TMS” sessions based on clinical needs after the initial round of treatments is completed.
For more information on TMS outcomes and ongoing support, you can explore resources on tms for ptsd and tms for bipolar depression. This comprehensive knowledge will aid you in making an informed decision about TMS therapy at MindHealth MD and its applicability to your situation.